Healthcare is moving toward personalization, but most systems still rely on fragmented data and reactive workflows. Patient records exist across EHRs, devices, and applications, yet translating that data into real-time, actionable insight remains a challenge.
AI is beginning to close this gap. By combining predictive models with unified data platforms, healthcare providers can shift from static records to continuously evolving patient intelligence, enabling earlier interventions and more tailored care decisions.
At the core of this approach is Amazon RDS, which provides a scalable and secure foundation for managing structured healthcare data. When integrated with AI pipelines, it becomes a critical component in building systems that support personalized care delivery at scale.
However, implementing such systems requires more than just choosing the right database. It involves designing modern data architectures, integrating AI workflows, and operationalizing insights, areas where experienced AWS partners like Mactores play a key role.
In this blog, we’ll break down how to build AI-powered patient intelligence using Amazon RDS and how it enables personalized care in real-world healthcare environments.
What is Patient Intelligence?
Patient intelligence is the process of transforming diverse patient data into meaningful, actionable insights that support clinical decision-making. In modern healthcare ecosystems, it goes beyond storing records; it enables a continuous, data-driven understanding of each patient’s condition, risks, and care needs.
At its core, patient intelligence brings together multiple data sources:
- Electronic Health Records (EHR): Medical history, diagnoses, lab reports, prescriptions
- Wearables and IoT streams: Real-time vitals such as heart rate, activity levels, and glucose monitoring
- Behavioral and demographic data: Lifestyle habits, age, location, and social determinants of health
While healthcare organizations generate vast amounts of data, much of it remains underutilized. The real challenge isn’t data collection, it’s turning that data into timely, actionable intelligence that clinicians can rely on.
This is where unified data platforms become critical. By consolidating and structuring data within systems like Amazon RDS, organizations can create a consistent foundation for analytics and AI. Ultimately, patient intelligence bridges the gap between raw data and better care outcomes.
The Role of AI in Personalized Care Delivery
AI is central to transforming fragmented healthcare data into predictive, actionable insights. By analyzing patterns across clinical records, real-time device data, and patient behavior, AI enables a shift from retrospective reporting to proactive care. Instead of relying on isolated data points, healthcare providers can build a connected, continuously evolving view of each patient, supporting earlier interventions and more precise treatment decisions.
In practice, AI powers several critical use cases. It helps identify at-risk patients before conditions worsen, supports clinicians with data-driven recommendations during diagnosis and treatment, and enables personalized therapies tailored to individual patient profiles. Beyond individual predictions, AI systems also evolve. As new data is generated, models can be retrained and refined, creating continuous learning systems that improve accuracy and relevance.
However, operationalizing AI in healthcare requires more than model development. It involves building robust data pipelines, ensuring model reliability, and integrating outputs into clinical workflows. This is where experienced AI teams, such as Mactores, contribute by developing production-ready systems that translate AI capabilities into real-world healthcare impact.
Why Amazon RDS is the Foundation for Patient Intelligence?
In healthcare architectures, Amazon RDS provides a managed and scalable foundation for storing structured patient data. It offers high availability, automated maintenance, and seamless integration with the broader AWS AI/ML ecosystem, making it well-suited for building patient intelligence systems. With built-in security features such as encryption and IAM, along with support for compliance requirements like HIPAA, it enables organizations to handle sensitive healthcare data reliably while focusing on deriving insights rather than managing infrastructure.
Data Modeling for Healthcare in Amazon RDS
Effective patient intelligence starts with how data is structured. In Amazon RDS, healthcare datasets must be modeled for both performance and scalability, ensuring that clinical queries, analytics, and AI pipelines can run efficiently on large, evolving datasets.
Key schema design considerations include:
- Patient-centric models: Organizing data around a unified patient entity to connect records like visits, diagnoses, and treatments
- Time-series data handling: Structuring continuous data from vitals, devices, and monitoring systems for efficient querying and analysis
To maintain performance at scale, optimization techniques are essential:
- Indexing: Speeding up access to frequently queried attributes (e.g., patient ID, timestamps)
- Partitioning: Managing large datasets by segmenting data logically (e.g., by date or patient groups)
- Query tuning: Refining queries to reduce latency and improve throughput
As healthcare systems grow, modernizing legacy database structures becomes critical to support these patterns, making data modeling a key enabler of scalable, AI-driven patient intelligence.
Integrating AI with Amazon RDS
Integrating AI with Amazon RDS involves building data pipelines that can reliably move and transform healthcare data into formats suitable for machine learning. ETL or ELT workflows extract data from RDS, enrich it through feature engineering, and feed it into ML services such as Amazon SageMaker for training and inference. These pipelines can support both batch processing, used for large-scale model training, and real-time inference for time-sensitive use cases like risk alerts or clinical decision support.
A critical aspect of this integration is creating feedback loops, where model predictions and new patient data are continuously fed back into the system to improve accuracy over time. Successfully implementing this requires aligning AI workflows with a well-architected data platform, combining data engineering and machine learning expertise to deliver reliable, end-to-end patient intelligence systems.
Enabling Personalized Care Workflows
Turning patient intelligence into real impact requires embedding AI directly into care workflows. This starts with segmenting patients into meaningful cohorts using clustering techniques, followed by risk scoring models that identify individuals who may need early intervention. Based on these insights, systems can generate dynamic care recommendations, ranging from treatment adjustments to preventive actions, tailored to each patient’s profile.
These outputs are then surfaced through clinician dashboards and decision support tools, ensuring that insights are accessible at the point of care. The goal is not just to generate predictions, but to make them usable within everyday clinical processes.
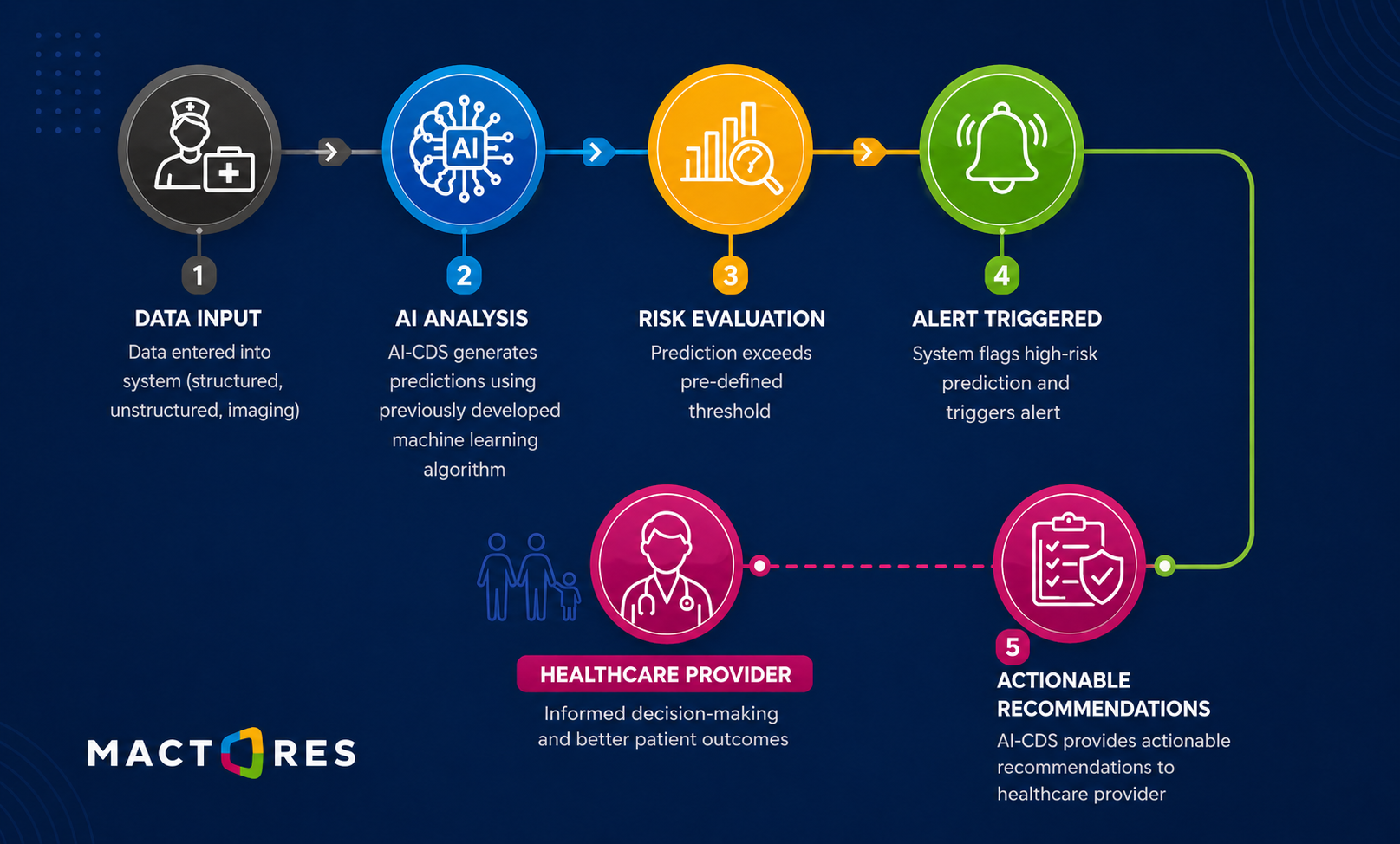
Operationalizing this end-to-end flow, data to insight to action, is what enables AI to move from experimentation to real-world healthcare delivery.
Getting Started: Implementation Roadmap
Building an AI-powered patient intelligence system requires a structured approach that aligns data, infrastructure, and clinical workflows. Rather than tackling everything at once, organizations should focus on incremental, outcome-driven implementation.
A typical roadmap includes:
- Define the use case: Identify a high-impact problem, such as readmission reduction or chronic disease monitoring
- Modernize data infrastructure: Set up a scalable foundation using Amazon RDS to manage structured healthcare data
- Build a unified data platform: Consolidate data from EHRs, devices, and external sources into a consistent model
- Develop and deploy AI models: Train models for prediction, segmentation, or recommendations based on the use case
- Integrate into workflows: Embed insights into clinician dashboards and care delivery systems
- Monitor and optimize: Continuously validate model performance and refine pipelines based on new data
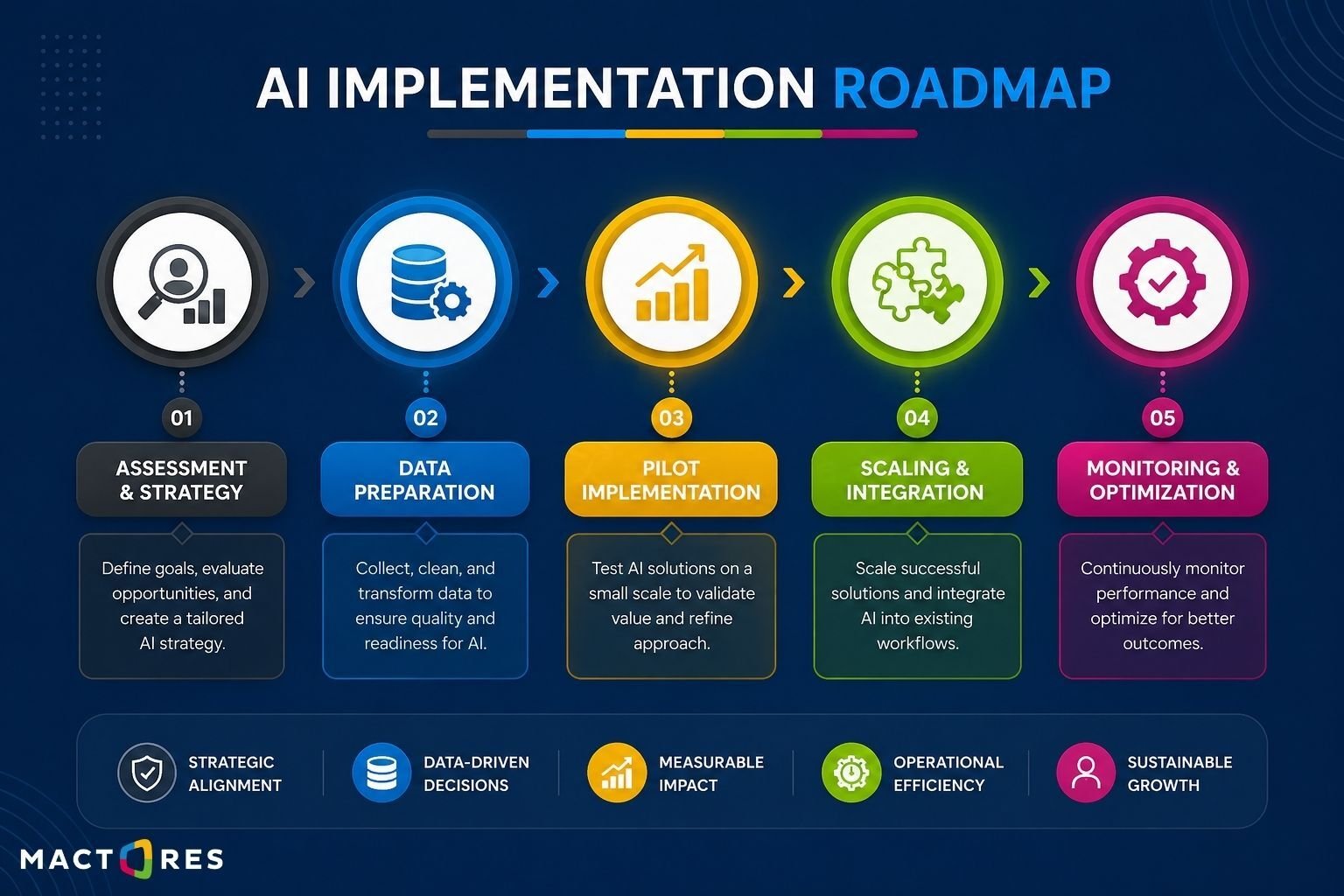
Executing this effectively often requires coordination across data engineering, AI development, and cloud architecture, making experienced AWS and AI teams valuable for accelerating delivery and reducing implementation risk.
Reducing Readmissions with AI-Powered Patient Intelligence
A healthcare provider managing chronic disease patients was struggling with fragmented data across EHR systems, remote monitoring devices, and care management platforms. This lack of integration made it difficult to identify high-risk patients early, resulting in frequent hospital readmissions, delayed interventions, and rising operational costs. Clinicians were often reacting to events rather than preventing them, limiting the effectiveness of care delivery.
To address this, Mactores designed and implemented an AI-powered patient intelligence platform built on Amazon RDS. The approach focused on unifying patient data, enabling predictive insights, and embedding those insights into clinical workflows.
Approach and Key Strategies:
- Unified data platform: Consolidated EHR, wearable, and historical patient data into a centralized RDS-backed architecture
- Patient segmentation: Applied clustering models to group patients based on risk profiles and disease patterns
- Predictive modeling: Built risk scoring models to identify the likelihood of hospital readmission and disease progression
- Real-time monitoring: Integrated streaming data from remote devices for continuous patient tracking
- Actionable insights: Delivered recommendations and alerts through clinician dashboards for timely intervention
- Feedback loop: Continuously retrained models using new patient data to improve accuracy
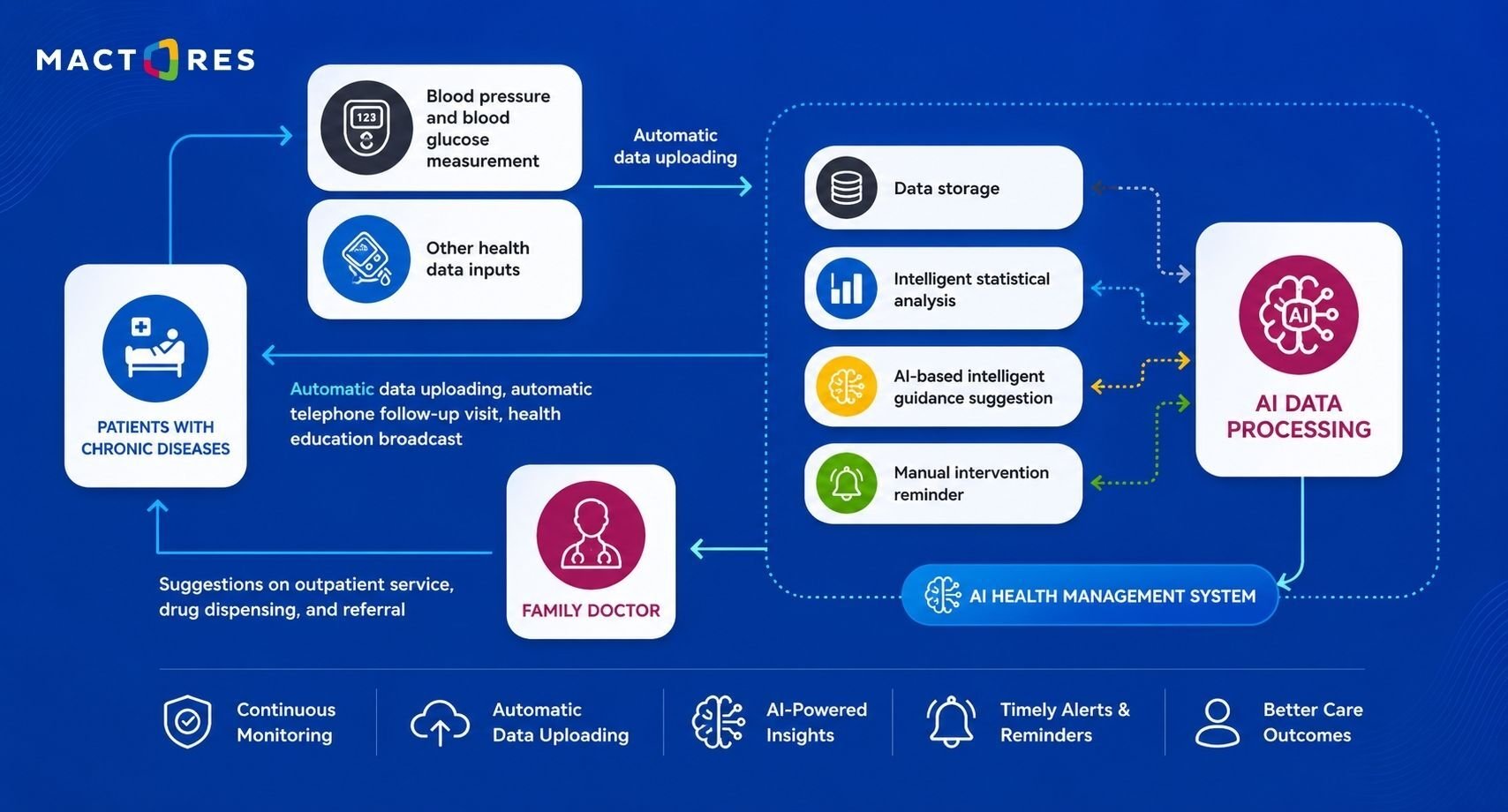
Outcomes Achieved:
- 30–40% reduction in hospital readmissions through early risk detection
- 25% improvement in care team response time due to real-time alerts
- 20% reduction in operational costs by minimizing emergency interventions and optimizing resource allocation
- Enhanced patient engagement via continuous monitoring and personalized care plans
This implementation demonstrates how enterprises can move beyond data collection to measurable outcomes by operationalizing AI within healthcare workflows.
Future of AI-Powered Healthcare
Healthcare is steadily moving toward systems that are not just data-driven, but intelligence-driven. Advances in generative AI are beginning to support clinical decision-making by summarizing patient histories, suggesting treatment pathways, and assisting with documentation. At the same time, agent-driven systems are emerging, where AI can autonomously monitor patient data, trigger workflows, and assist in care coordination with minimal human intervention.
Privacy and interoperability remain central to this evolution. Approaches like federated learning allow models to learn from distributed datasets without exposing sensitive patient information, while standards such as FHIR and HL7 are enabling more seamless data exchange across healthcare systems.
Together, these advancements point toward a shift from isolated applications to connected, intelligent ecosystems, where data platforms, AI models, and applications work in sync. As organizations adopt these capabilities, healthcare delivery will increasingly move toward autonomous, continuously optimizing systems that improve outcomes while reducing operational complexity.


